Reviewed by Thomas Watson, RRCA-certified running coach & Marathon Handbook founder.
Key Takeaways
Achilles tendonitis is one of running most stubborn injuries — a degenerative condition more than an inflammatory one. The fix is eccentric calf-loading (the Alfredson protocol), gradual return to running, and addressing the biomechanical issues that caused it in the first place.
Are you noticing pain or sensitivity in the back of your lower leg?
The Achilles tendon is a common area of injury in runners, with Achilles tendonitis for runners claiming the throne as the second-most common running-related musculoskeletal injury with a staggering incidence rate of 9.1% to 10.9%.
Achilles tendonitis for runners can get progressively worse if left untreated and may end up leaving you unable to run for a significant period of time. For this reason, effective treatment requires adherence to a structured rehab program.
This article will provide up-to-date science regarding Achilles tendonitis for runners, giving you the tools to help evaluate and treat this problematic injury.
Achilles was a fearless hero who suffered defeat due to the vulnerability of his Achilles heel. Keep reading as we discuss the following and ensure you avoid the same mistakes he did:
- What Is Achilles Tendonitis For Runners?
- Causes of Achilles Tendinopathy
- Achilles Tendinopathy Symptoms and Diagnosis
- Can You Run With Achilles Tendinopathy?
- How To Effectively Treat Achilles Tendinopathy
Let’s jump in!

What is Achilles tendonitis For Runners?
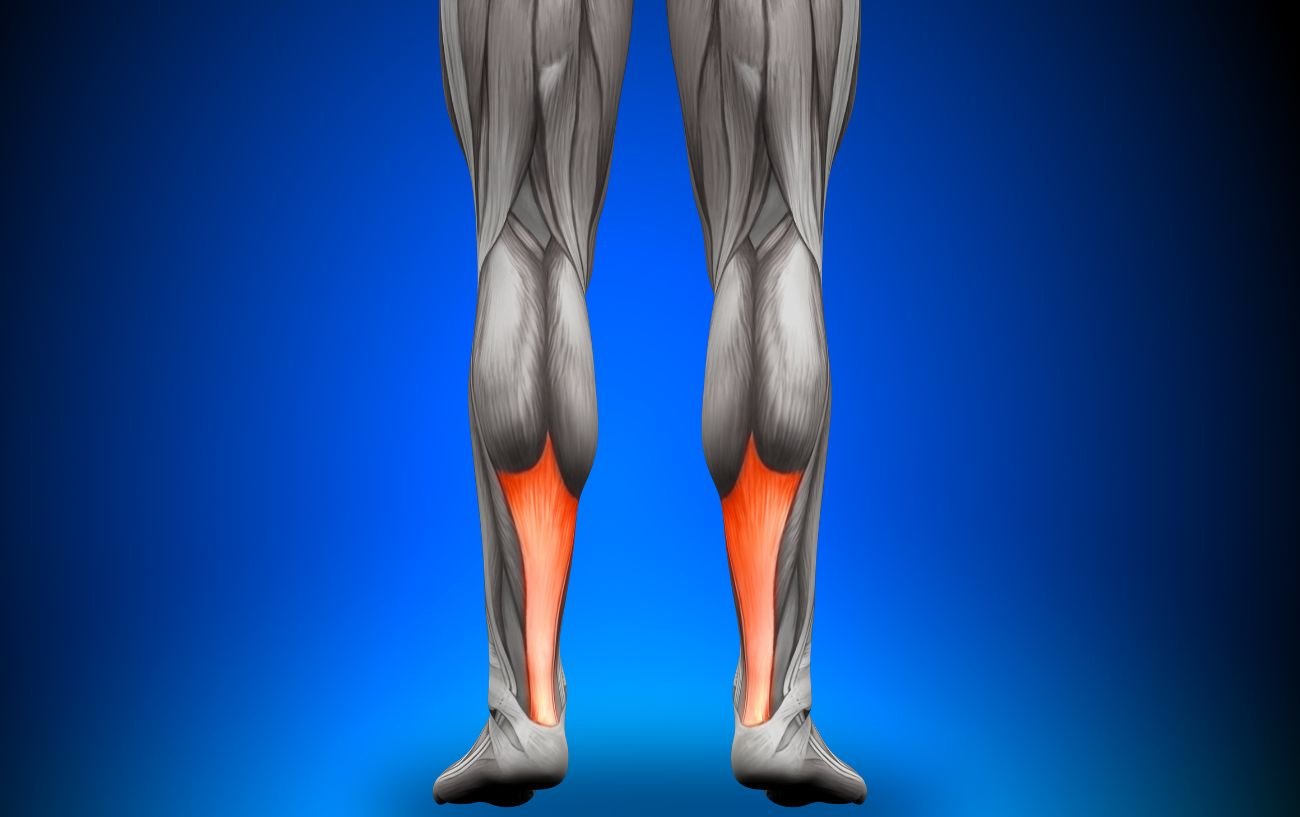
The Achilles tendon is the strongest tendon in the human body. It helps your foot flex and is responsible for your ability to walk, run, jump, and stand.
The tendon has the capacity to resist large tensile forces. It connects the gastrocnemius and soleus muscles to the calcaneus (heel).
The condition is more accurately described as Achilles tendinopathy, as ‘itis’ refers to inflammation, which is not always present. Instead, the actual cause is physical damage and degeneration of the collagen fibers of the Achilles tendon itself.
Achilles tendinopathy is often a result of over-use, in which excessive compression during repeated energy storage and release results in unmanageable stress upon the tendon.
Over time, if untreated, the tendon can get tighter and weaker, leading to sudden injury and rupture.
There are two types of Achille’s tendonitis:
- Insertional Achilles tendinopathy refers to damage in the lower part of the tendon, where it attaches to your heel. Compression is considered a critical factor in insertional tendinopathy.
- Non-insertional Achilles tendinopathy is damage in the middle of the tendon. Tensile loading is considered a critical factor in non-insertional tendinopathy.
It is helpful to further break down the degrees of tendinopathy you may experience. Cook and Purdum proposed that there are three stages:
Stage 1: Reactive Tendinopathy
A reactive tendon is a non-inflammatory proliferative response by the cells. This is a result of compressive or tensile overload. During this phase, the tendon thickens to reduce stress and increase stiffness. The tendon can have the potential to revert back to its normal state.
Stage 2: Tendon Disrepair
This stage is often the natural progression from reactive tendinopathy if you continue to overload the Achilles frequently. During this stage, there is increased vascularity and protein production within the tendon, although the result is more stiffness and less adaptivity.
Stage 3: Degenerative tendinopathy
The tendon has a poor prognosis at this stage, with most of the changes now irreversible. Cell death is present in the tendon. Often seen in the older population and younger adults who have continually excessively overloaded.

Causes of Achilles Tendinopathy
As previously mentioned, Achilles tendinopathy is a result of excessive stress being transmitted through the tendon. The most common cause is overuse and subsequent tendon overload.
Certain causes, such as weak calf muscles, excessive pronation, and poor ankle range of motion, have all been connected with the development of Achilles problems.
Other known risk factors include:
- Obesity
- High blood pressure
- Rapid changes to load volume
- Type II Diabetes
- Family history of tendinopathy
- Inappropriate running shoes
Achilles Tendinopathy Symptoms & Diagnosis
To accurately diagnose Achilles Tendinopathy, consult a medical professional.
You will usually be able to observe the loss of muscle (atrophy), swelling, asymmetry, and redness of the skin, also known as erythema.
Palpation of the tendon may cause localized tenderness.
You may also experience loss of range of motion, particularly during ankle dorsiflexion (toes up) and heel raises.
Can you run with Achilles tendinopathy?
The answer is not a straightforward yes or no, and whether you can, will often differ from whether you should.
The first port of call should be to take a few days off running. That way, you can take stock of the pain and make an informed decision.
Most people find that their symptoms begin to improve within 12 weeks. However, the risk of re-aggravation is high. You have the power to influence recovery time through your active participation in the recovery process.
The most common mistake runners make is jumping back into running too quickly.
You can run only if your Achilles does not aggravate before, during, or after. The likelihood is that if you’re suffering from acute tendinopathy and you feel pain when walking or as soon as you start running, your body could probably do with some rest.
Continuing to run with Achilles tendinopathy may slow the healing process and prolong the course of the injury.
However, injury isn’t straightforward, and the body can often deal with low loads when aggravated.
If you have non-acute Achilles tendinopathy, complete rest is not necessary.
If the symptoms are mild and don’t deteriorate with exercise, then a substantially reduced volume of running is certainly possible.

How to effectively treat Achilles Tendinopathy
The specific program of rehabilitation you should follow for your Achilles tendinopathy will depend on a number of factors, which is why you should seek out the help of a medical professional.
Factors such as whether it is insertional or non-insertional, alongside the degree of tendon damage, should be considered when undergoing rehab.
Rehab should be comfortable; at no point do you need to put the body under excessive stress. As we continue to exercise, we increase our body’s capacity for load/stress.
Take your time; progression is a process. What was an uncomfortable exercise two weeks ago may now feel comfortable. That is our capacity increasing.

Phase 1: Reducing Pain
If your injury is acute, you can use the RICE method (rest, ice, compression, and elevation) to help treat your pain right away.
Rest – Try to keep off your foot for as much as possible. Again, this includes no running for a few days!
Ice – Apply ice, or some type of cold compress, to the area for 20 minutes at a time, three times a day. This can help reduce pain in the area.
Compression – You can wear some type of compression garment around your tendon to increase blood flow. This will reduce swelling. You can use compression socks, bandages, or tape to wrap the area.
Elevate – Finally, take a load off and elevate your foot. You want it to be above the level of your chest if possible, so you may need to lay down and prop your foot on a pillow. The goal is to keep the blood from pooling in your ankle and get it back to your heart as quickly as possible to reduce swelling.
Isometric tendon loading is a well-researched tool for tendinopathy treatment.
Isometric tendon loading has been found to have pain-relieving effects on tendons while simultaneously maintaining some baseline strength.
An isometric calf raise is a great exercise to utilize
Push yourself onto your toes for 40-60 second holds, and repeat 4-5 times.
If the tendon is highly irritable, try both feet down, holding for a shorter time or fewer repetitions.
Phase 2 – Improve Strength
What loading level is appropriate for you depends on the stage and severity of your condition and how confident you are with resistance training.
Aim to exercise with sufficient load in a muscle’s mid-range position. Avoid exercising with heavy loads in positions where there is likely to be tendon compression.
Eccentric (lengthening) exercises have been considered the gold standard for tendon rehab since research by Alfredson et al. (1998). More recently, research has highlighted the importance of including the concentric (shortening) phase of exercises with heavy, slow resistance training
Promising Achilles tendinopathy rehab was seen during Jonsson et al. (2008), where an eccentric loading program was used. However, they avoided loading into dorsiflexion.
Heavy, slow resistance training should be practiced in the mid-range of the movement.
According to Kongsgaard et al. (2010), a heavy, slow resistance program may look like this:
Four sets of 15-6 reps, which started with 15 rep max and progressed to 6 rep max over a period of 12 weeks.
Try a six-second calf raise, 3 seconds up, 3 seconds down. Adding weight when required.
What is heavy will change as your strength builds; the prescribed exercise should be challenging without eliciting pain from the tendon.
Phase 3 – Functional Rehabilitation
By this point, you may have already re-introduced running. A gradual return to usual activities, alongside a strength phase, will often be enough to rehabilitate tendinopathy.
However, running induces a high level of impact. During the running cycle, the tendon’s Stretch-Shortening-Cycle is activated. Avoid re-aggravation with adequate muscle strength.
Therefore, functional rehabilitation is recommended.
A plyometric jump squat is a great exercise that will begin to mimic the forces the Achilles will eventually be subjected to.
Try three sets of 15 repetitions.
Remember, it is always important to check with your healthcare professional to properly diagnose your injury and create an actionable plan with appropriate exercise for your individual situation to jump-start your rehab!
For some at-home leg-strengthening exercises, click here.
Frequently Asked Questions
Can I keep running with achilles tendonitis?
Sometimes. If pain is below 3 out of 10 and does not worsen during the run or in the 24 hours after, you can typically run through it with reduced volume. Sharp pain, swelling, or morning stiffness lasting more than 30 minutes means stop running and rehab.
How long does achilles tendonitis take to heal?
Most cases need 6-12 weeks of consistent eccentric calf strengthening. Chronic cases (more than 6 months symptomatic) often take 4-6 months to fully resolve and may need shockwave therapy or PRP injections in stubborn cases.
What is the Alfredson protocol for achilles tendonitis?
Three sets of 15 eccentric heel drops on a step, twice a day, for 12 weeks. Half the sets with a straight knee (gastrocnemius), half with a bent knee (soleus). Research shows it resolves 80%+ of cases without surgery.
Should I use ice or heat on achilles tendonitis?
Heat for chronic stiffness (most common in runners), ice only for acute flares with swelling. Achilles tendinopathy is not primarily inflammatory in chronic cases, so ice does not speed recovery — but heat improves blood flow to a poorly vascularized tendon.
Are heel raises in my shoes useful for achilles tendonitis?
Yes, temporarily. A 6-12mm heel insert reduces strain on the tendon and is useful for the first 4-6 weeks of rehab. Wean off them as strength returns or you risk shortening the calf chain.












