Injury prevention for runners’ feet doesn’t start and end with buying a good pair of shoes. While the right running shoes are incredibly important—they are, after all, the only thing between your feet and miles of unforgiving pavement—there’s much more to keeping your feet healthy.
One study that followed 1,680 runners over a year found that nearly half—48%—experienced at least one injury during that time. Of those injuries, 54% were new, while the rest were recurrences of previous problems that had never fully resolved.1Walter, S. D. (1989). The Ontario Cohort Study of Running-Related Injuries. Archives of Internal Medicine, 149(11), 2561. https://doi.org/10.1001/archinte.1989.00390110113025
Too often, runners try to “run through” minor foot issues or simply give them time to heal, allowing small irritations to turn into persistent injuries that can disrupt weeks—or even months—of training.
Running places significant stress on the feet with every stride as they absorb impact, stabilize movement, and propel the body forward. Over time, this repetitive load can lead to a range of problems, from skin irritations to tendon inflammation.
Fortunately, many of the most common foot issues runners face are both preventable and treatable with the right habits, equipment, and attention to early warning signs.
We’ll take a closer look at the five most common foot ailments runners encounter—including Achilles tendonitis, athlete’s foot, friction blisters, runner’s toe, and plantar fasciitis—along with practical ways to treat them and prevent them from returning.
We’ll also cover general foot care habits that can help keep your feet healthy and ready for the miles ahead.
The 5 Foot Injuries Most Runners Deal With
#1: Achilles Tendonitis

The Achilles tendon is the largest tendon in the human body, connecting your calf muscles to your heel bone. It plays a critical role in nearly every lower-body movement, allowing you to walk, run, jump, and push off the ground with each stride.
Because this tendon handles so much force during daily activities—especially running—it’s easy to see why injuries to the Achilles can be particularly disruptive for runners.
Achilles tendonitis occurs when this tendon becomes irritated and inflamed. The inflammation typically develops in one of two locations along the tendon.
When it occurs at the tendon’s attachment to the heel bone, it is known as insertional Achilles tendonitis. When the irritation develops higher up along the tendon, usually in the middle portion, it is referred to as non-insertional Achilles tendonitis.
Regardless of the location, Achilles tendonitis often presents with pain and swelling along the back of the heel or lower calf, along with tightness in the calf muscles and a reduced range of motion when flexing the foot.
Many runners also notice stiffness first thing in the morning or at the beginning of a run, which may gradually improve as the tendon warms up.
What Causes Achilles Tendonitis?
In most cases, Achilles tendonitis comes down to overuse—plain and simple.
The Achilles tendon absorbs a tremendous amount of stress with every step you take, helping transfer force from your calf muscles to your foot.
When the workload placed on this tendon increases too quickly, whether from higher mileage, faster workouts, or more frequent runs, it can become irritated and inflamed.
This is why gradually increasing your training volume is so important. Doing too much too soon can place excessive strain not only on your Achilles tendon but on your entire lower leg.
Several common training habits can contribute to Achilles tendon overuse, including:
- Worn-out running shoes, which no longer provide proper cushioning and support
- Skipping a proper warm-up, leaving the calves and Achilles tight and unprepared for impact
- Sudden increases in training volume or intensity
- Poor running mechanics or inefficient form
Over time, these factors can combine to overload the tendon, leading to pain, stiffness, and reduced performance if not addressed early.
How To Treat Achilles’ Tendonitis
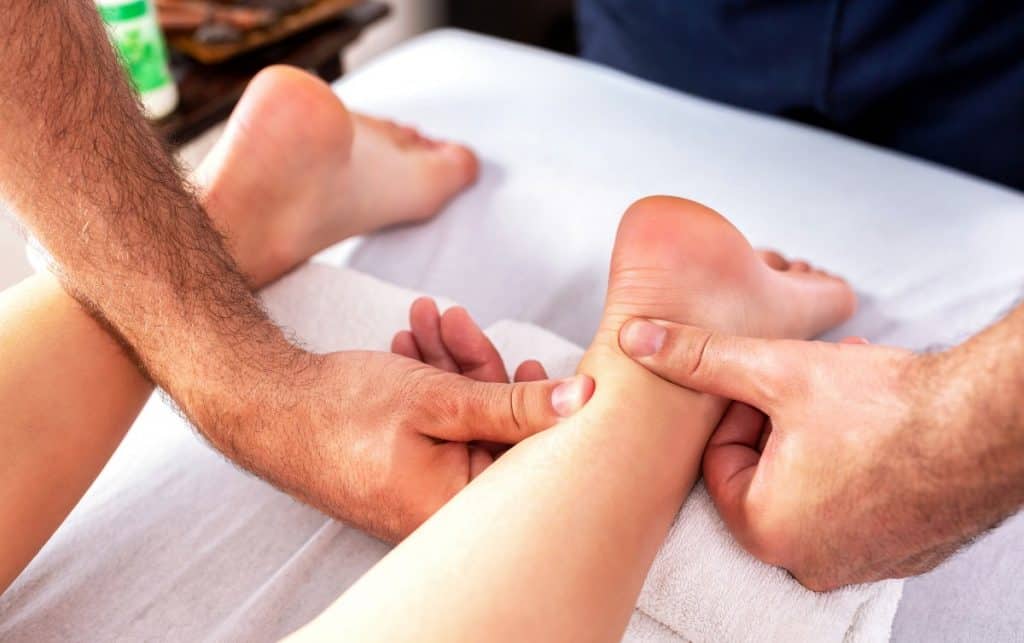
The most important first step in treating Achilles tendonitis is reducing the load on the tendon to allow it to heal.
Continuing to run through pain often worsens the inflammation and can turn a mild issue into a chronic injury. In most cases, giving the tendon time to calm down—combined with a few simple recovery strategies—can significantly speed up the healing process.
A helpful starting point is the classic RICE method: Rest, Ice, Compression, and Elevation.
Rest:
Give the tendon a break from running and high-impact activities for several days, or longer if symptoms are more severe. Low-impact cross-training such as cycling, swimming, or using the elliptical can often help maintain fitness without placing as much stress on the Achilles.
Ice:
Applying ice helps reduce inflammation and pain. Hold an ice pack or a bag of frozen vegetables on the affected area for 15–20 minutes at a time, two to three times per day, especially after activity.
Compression:
Compression socks, sleeves, or wraps can help reduce swelling and support circulation in the lower leg. Many runners find compression useful during recovery and when gradually returning to training.
Elevation:
When resting, elevate your foot above heart level if possible—for example, lying down with your leg propped up on pillows. This helps limit swelling and encourages fluid drainage from the area.
Beyond the RICE method, several additional strategies can support recovery:
- Gentle calf stretching once the acute pain settles can help relieve tension on the tendon.
- Eccentric calf strengthening exercises (like slow heel drops) are widely recommended by physical therapists to help rebuild tendon strength and resilience.
- Checking your running shoes is also important; worn-out or unsupportive shoes can increase strain on the Achilles.
- Gradually returning to running is key—avoid jumping right back into high mileage or speed workouts.
If pain persists for more than a couple of weeks, becomes severe, or interferes with walking, it’s wise to consult a physical therapist or sports medicine professional. Early guidance can help prevent the issue from progressing into a long-term injury.
#2: Athlete’s Foot

Athlete’s Foot, also called tinea pedis, is a fungal infection often found between the toes. When it happens, you’ll most likely have a scaly rash that can itch, sting, or burn. It can also cause blisters, ulcers, or cracking and peeling skin.
What Causes It
This fungus is contagious and thrives in moist environments such as damp floors and wet socks. It’s commonly found in locker rooms, showers, and swimming pools.
How to Treat Athlete’s Foot
Since it’s a fungal infection, it usually won’t resolve on its own without treatment. The good news is that it’s typically easy to manage if you catch it early.
The first line of treatment is usually an over-the-counter topical antifungal medication, available at most drugstores. These creams, sprays, or powders work by killing the fungus and preventing it from spreading.
Apply the medication as directed—usually once or twice per day—and continue using it for the full recommended period, even if symptoms start to improve quickly.
If the infection doesn’t improve after a couple of weeks, or if it spreads or becomes painful, it’s a good idea to consult a doctor, who may prescribe a stronger antifungal medication.
Prevention is especially important with athlete’s foot because the fungus thrives in warm, moist environments, which runners frequently create inside their shoes during long workouts. Taking a few simple steps can significantly reduce your risk:
- Wear moisture-wicking synthetic running socks designed to keep your feet dry and comfortable.
- Change out of sweaty socks immediately after your run to prevent moisture from lingering on your skin.
- Wash your feet regularly and dry them thoroughly, especially between the toes, where fungus tends to develop.
- Allow your running shoes to dry completely between runs. Rotating between two pairs of shoes can help each pair air out.
By keeping your feet clean, dry, and well cared for, you can greatly reduce the chances of athlete’s foot interrupting your training.
#3: Friction Blisters
You’ve undoubtedly had a few of these at some point throughout your life. These are those uncomfortable, often painful, raised bumps on the skin.
They fill with fluid, often found after a long day of walking around.
Blisters are your body’s way of forming a cushion between you and further injury, and are even more common in runners’ feet.
What Causes Them
Repetitive friction and rubbing.
In fact, blisters need three things to propagate: heat, moisture, and friction. All of these three can show up quickly in your running shoes.
Often, poor-quality socks or ill-fitting running shoes are guilty here.
Make sure you choose the right running shoe size and shape for your feet, and that they’re suited for the type of running you do most often.
5 Ways to Prevent Friction Blisters

Friction blisters are one of the most common—and frustrating—issues runners face. They occur when repeated rubbing causes the outer layer of skin to separate from the layers beneath it, allowing fluid to collect and form a blister.
Fortunately, a few simple preventative habits can go a long way toward keeping your feet blister-free.
- Replace your running shoes regularly. As shoes wear down, they can begin to move differently on your foot, creating new pressure points. A general guideline is to replace running shoes every 300–500 miles, though this can vary by shoe and running style.
- Wear moisture-wicking socks that fully cover your feet. Quality running socks help create a protective barrier between your skin and the inside of your shoe while also reducing moisture buildup.
- Use adhesive cushion pads or blister tape on areas where you frequently notice rubbing, such as the heel or the sides of your toes. These can help reduce friction before it becomes a problem.
- Use lubrication. Applying an anti-chafing balm or a small amount of petroleum jelly (like Vaseline) to high-friction areas can help minimize rubbing during longer runs.
How to Treat Friction Blisters When It’s Too Late for Prevention
The good news is that most friction blisters heal on their own within a few days if they’re left protected and clean. The fluid-filled pocket typically begins to shrink, and the skin underneath starts to repair itself within a day or two.
As tempting as it may be, try not to pop the blister.
The skin covering the blister acts as a natural protective barrier against infection. If a blister does rupture on its own, gently clean the area with soap and water, apply an antibiotic ointment, and cover it with a sterile bandage or blister pad to keep it protected while it heals.
If you want a deeper dive into blister prevention and treatment strategies, be sure to check out our full guide on dealing with blisters for runners.
#4: Runner’s Toe

Runner’s toe, also known as subungual hematoma or jogger’s toenail, occurs when repeated impact during running causes small blood vessels beneath the toenail to break. Blood then collects under the nail plate, creating pressure and discoloration in the nail bed.
This usually happens when the toe repeatedly hits the front of the shoe during downhill running, speed workouts, or long runs where the foot slides forward inside the shoe. Over time, this constant micro-trauma can damage the nail bed and surrounding tissue.
The most noticeable symptom is that the toenail begins to turn dark red, purple, or black, which can look alarming if you’re not familiar with the condition.
The area may feel tender or sore, especially when pressure is applied to the nail. If enough blood accumulates beneath the nail, the pressure can cause the nail to lift away from the nail bed. In some cases, the damaged nail will eventually loosen and fall off completely.
While losing a toenail might sound dramatic, it’s actually a relatively common experience among runners, particularly marathoners and ultrarunners. In most cases, the nail will grow back over time, though it can take several months for a new nail to fully replace the old one.
What Causes It
Runner’s toe typically develops when your toes repeatedly hit or press against the front of your shoe’s toe box during running. This impact might not feel like a big deal at first, but over the course of hundreds or thousands of strides, that constant pressure can damage the small blood vessels under the nail.
The first few taps might not hurt at all, but after dozens or hundreds of repetitions, the tissue becomes irritated and eventually bruised.
Several factors can increase the risk of runner’s toe, including shoes that are too small, downhill running, long-distance races, and feet sliding forward inside the shoe due to loose lacing or worn-out footwear.
How to Treat Runner’s Toe

The good news is that runner’s toe is usually not serious and often heals on its own. If there’s little or no pain and the nail is simply discolored, the best approach is often to leave it alone and allow the body to recover naturally.
However, if there is significant pain or pressure beneath the nail, it may indicate that too much blood has collected under the nail bed. In this case, a medical professional may drain the fluid to relieve pressure.
This procedure should always be performed by a doctor or healthcare provider—never attempt to do it yourself, as improper treatment can lead to infection.
If the damaged toenail eventually loosens and falls off, don’t panic. This is fairly common among runners. Often, a new nail is already beginning to grow underneath.
Keep the exposed area clean and protected by applying an antibiotic ointment and covering it with a bandage while it heals. If you notice excessive pain, swelling, or signs of infection, it’s best to have a doctor examine the toe to ensure everything is healing properly.
Read our full guide to dealing with Runner’s Toe
#5: Plantar Fasciitis
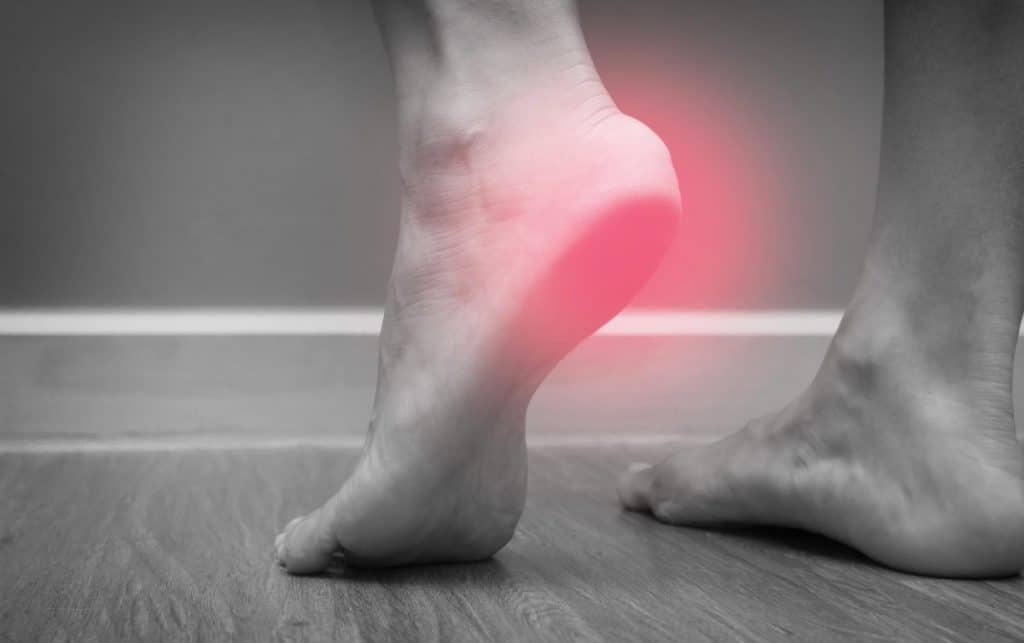
Plantar fasciitis is one of the most common foot injuries among runners. It occurs when the plantar fascia, a thick band of connective tissue that runs along the bottom of your foot from your heel bone to your toes, becomes irritated or inflamed.
This tissue plays a critical role in supporting the arch of your foot and helping absorb the impact forces generated with every step. It also acts like a spring, storing and releasing energy as you walk or run.
The most common symptom of plantar fasciitis is sharp pain in the heel or along the arch of the foot. Many runners notice it most strongly first thing in the morning when they take their first few steps out of bed, or after standing up following a long period of sitting.
This happens because the plantar fascia tightens at rest, and the first steps place sudden stress on the irritated tissue. The pain may ease somewhat as you move around and the tissue warms up, but it often returns after long runs or prolonged time on your feet.
While frustrating, plantar fasciitis is usually manageable with the right combination of rest, stretching, strengthening, and gradual return to running. Addressing it early is key, as ignoring the symptoms can allow the irritation to worsen and extend recovery time.
What Causes It
Plantar fasciitis is most often the result of repetitive stress and overuse on the plantar fascia. Because this tissue absorbs impact and helps stabilize the foot’s arch, it experiences significant strain during running.
When the load placed on it exceeds what the tissue can comfortably handle, tiny micro-tears can develop, eventually leading to irritation and inflammation.
For runners, the most common cause is increasing training volume or intensity too quickly. Adding extra mileage, introducing speed workouts, or running more hills than usual can overload the plantar fascia before it has time to adapt.
Several other factors can also contribute to plantar fasciitis, including:
- Tight calf muscles or Achilles tendons, which increase tension on the plantar fascia
- Poor footwear or worn-out running shoes that no longer provide adequate support or cushioning
- High arches or very flat feet, both of which can place extra stress on the fascia
- Running on hard surfaces for long periods, such as pavement or concrete
- Weak foot, ankle, or hip muscles, which can alter biomechanics and increase strain on the bottom of the foot
Often, plantar fasciitis develops not from a single cause but from a combination of training errors, muscle tightness, and footwear issues. Identifying and addressing these underlying factors is key to both treating the injury and preventing it from returning.
How to Treat Plantar Fasciitis

Treating plantar fasciitis usually begins with reducing the stress on the plantar fascia so the tissue has time to calm down and heal.
This often means temporarily cutting back on running mileage or taking a short break from high-impact activities, especially if the pain is sharp or worsening. During this time, many runners maintain their fitness by switching to low-impact cross-training, such as cycling or using the elliptical.
One of the most effective treatments is consistent stretching and strengthening, particularly for the calves, Achilles tendon, and foot muscles. Tight calves increase tension on the plantar fascia, so regular calf stretching can help reduce strain on the tissue.
Rolling the bottom of the foot with a massage ball, frozen water bottle, or foam roller can also help relieve tension and improve blood flow to the area.
Footwear also plays an important role in recovery. Wearing supportive shoes throughout the day, rather than walking barefoot on hard floors, can reduce irritation while the fascia heals.
In some cases, runners benefit from arch supports, orthotics, or taping techniques that help offload stress from the plantar fascia.
Most cases improve gradually with these conservative treatments, but if pain persists for several weeks, it may be helpful to consult a physical therapist or sports medicine professional.
Early guidance can help address underlying causes such as muscle imbalances, tightness, or training errors, allowing you to return to running safely and prevent the injury from recurring.
Tips to Care for Your Feet
Taking care of your feet is one of the simplest ways to prevent injuries and keep your training consistent. A few proactive habits can go a long way toward keeping you comfortable and running smoothly.
- Pay attention to your running form. Efficient mechanics help distribute the workload across the correct muscles and reduce unnecessary stress on your feet and lower legs.
- Use the right gear. Proper running shoes, moisture-wicking socks, anti-chafing products, and blister-prevention tools can all make a big difference in protecting your feet during long runs and workouts.
- Never skip your warm-up or cooldown. Simple mobility and activation exercises—such as toe raises, calf stretches, and heel drops off a step—can prepare your feet and calves for the demands of running and help maintain flexibility.
- Take care of your skin. Keeping the skin on your feet moisturized can prevent dryness and cracking, which may otherwise lead to discomfort or infection. Applying lotion regularly can help maintain healthy skin.
- Monitor your training load. A common thread among many running injuries is overuse. While increasing mileage can improve fitness, it’s important to progress gradually. Keeping a training log and following the 10% rule—increasing your weekly mileage by no more than 10%—can help reduce the risk of overloading your feet.
Finally, if you notice persistent pain, unusual swelling, or anything that doesn’t seem right, it’s always best to consult a medical professional. Addressing issues early can help prevent small problems from turning into long-term injuries.











