Running a marathon is hard on the body, especially the heart. But what really happens physiologically after running 26.2 miles, and what might predict a larger post-race rise in cardiac biomarkers?
A new study directly addresses that question1Siekierzycka, A., Radulska, A., Woźniak, M., Pelikant-Małecka, I., Janaszak-Jasiecka, A., Lewicka, E., Kalinowski, L., & Olek, R. A. (2024). Plasma cardiovascular stress biomarkers response to marathon running. Sports Medicine and Health Science, 7(6), 481–486. https://doi.org/10.1016/j.smhs.2024.11.005 using blood biomarkers associated with cardiac stress and vascular strain. The researchers weren’t just looking at the average runner response. They asked whether a gut-derived metabolite called TMAO (short for trimethylamine-N-oxide)—a compound linked in other contexts to cardiovascular risk—might identify runners who show a bigger spike in “cardiac stress” markers after the race.

They recruited 28 healthy male amateur marathoners (no known history of disease) who were running a sea-level marathon in northern Poland. Blood samples were taken at three time points: two weeks before the marathon, immediately after finishing, and two weeks after.
They measured a panel of biomarkers, including:
- Cardiac troponin I (cTnI): the famous “heart muscle injury” marker (though it can rise after hard endurance exercise without a heart attack).
- Endothelin-1 (ET-1): a potent vasoconstrictor linked to vascular stress and blood pressure regulation.
- Inflammatory and stress-related markers like galectin-3, pentraxin-3, GDF-15, plus white blood cell counts and immune ratios.
They then divided runners into two groups based on baseline TMAO levels: Low TMAO (<4.0 μM; n=18) and High TMAO (≥4.0 μM; n=10). Training volume and marathon time were similar between groups (both averaged around ~4 hours).
The marathon elevated a bunch of biomarkers—cardiac, vascular, and inflammatory—right after the finish, and most of them settled back down by two weeks. Where it gets interesting is when we look at who saw more of a “spike” after the race.
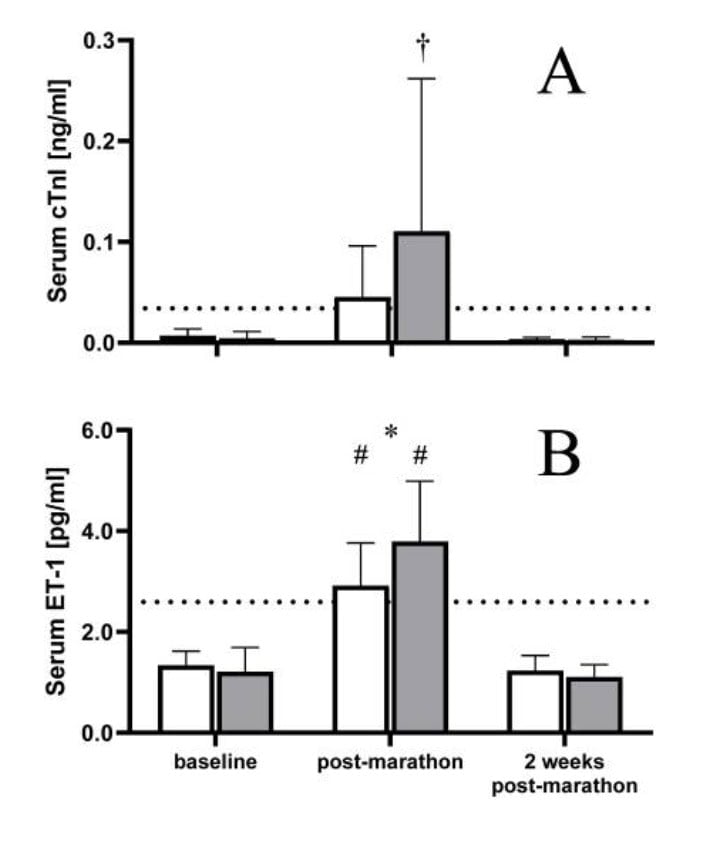
The high-TMAO group showed a clearer post-marathon rise in cTnI. The paper notes that post-race cTnI values were above a commonly used clinical cutoff for men (0.034 ng/mL) and that this rise was more pronounced in the high-TMAO group. Even more telling was that baseline TMAO was positively related to how much troponin increased from baseline to post-race (the higher your starting TMAO, the bigger your troponin bump).
ET-1 jumped in both groups after the marathon, but the high-TMAO runners had higher ET-1 immediately post-race than the low-TMAO runners. Baseline TMAO was also associated with the magnitude of the ET-1 increase. Post-marathon ET-1 levels exceeded the reference cutoff cited by the authors (2.59 pg/mL) and returned to baseline by two weeks.
The marathon also triggered a classic immune response—white blood cells roughly tripled, with neutrophils surging and lymphocytes dipping. But these inflammatory changes did not differ meaningfully between low- and high-TMAO groups. Thus, TMAO appeared to relate more to the troponin/ET-1 story than to the broader immune surge.
TMA (the precursor to TMAO) increased after the marathon, which the authors discuss as a possible hint of short-term gut permeability changes during and after endurance racing. But TMAO itself didn’t change much across time points—it was the baseline level that mattered for predicting the biomarker spike.
What this means for runners
If there’s a practical takeaway here, it’s that post-marathon “cardiac stress” signals aren’t one-size-fits-all. Two runners can train similarly and run similar times, yet one may exhibit a greater troponin and vascular strain response, and baseline TMAO levels might be a clue as to which runner is which.
I wouldn’t use this to spiral about your gut microbiome after every long run, but it does reinforce a couple common-sense approaches: respect recovery after marathons (because the internal stress response is real even when you “feel fine”), build durability gradually so the race isn’t a shock to the system, and pay attention if you’re someone who repeatedly has outsized physiological reactions to very long hard efforts. This paper nudges us toward a more individualized view of marathon stress.