Most runners consider their extremely low resting heart rate (medically referred to as bradycardia) a badge of honor. After all, it’s the result of years or even decades of hard work and thousands of miles logged.
My true overnight resting heart rate is somewhere between 32 and 35 beats per minute, and it’s been 40 beats per minute or below for as long as I can remember. Perhaps you’ve experienced something similar—a heart rate in the 30s or 40s that you’ve long attributed to endurance training alone. Endurance athletes understand it. It’s normal. Most mere mortals see the number and get concerned.
Well, according to recent evidence, there may be nothing to be worried about. More importantly, the research suggests that an extremely low heart rate may not just result from strenuous endurance training, but also from an underlying genetic predisposition.
A new Circulation paper is the most satisfying kind of research for athletes who like data. It asks how common bradycardia is, how extreme it presents, what else shows up on monitoring, and—most interestingly—how much of this might be baked into your genetics rather than earned purely through training.

Sinus bradycardia (a slow heart rhythm originating from the sinus node or SA node of the heart) is a classic “athlete’s heart” feature. Historically, we’ve debated the mechanisms: is it mostly high vagal tone (more parasympathetic “brake”), or is the sinus node itself remodeled by years of endurance training? This new study adds a third lever—inherited biology. And it’s absolutely fascinating (to me, and hopefully to you).
The authors used a validated heart-rate polygenic risk score (which I’ll refer to from here on out as HR-PRS)—basically, a large bundle of common genetic variants that, in aggregate, predict a lower or higher heart rate. If genetics meaningfully contribute to athletic bradycardia, then athletes with a lower heart rate “genetic signature” should be overrepresented among the most bradycardic, and potentially among endurance athletes in general.
Researchers studied 465 current and former elite endurance athletes from the Pro@Heart/ProAFHeart cohorts (median age 23, 75% men). Sports were mostly cycling (37%), rowing (34%), running (16%), and triathlon (10%). Everyone underwent the following tests:
- A 24-hour Holter monitor (with athletes told to live/train normally) to continuously measure heart rhythm.
- Resting ECG
- Cardiopulmonary exercise testing (cycle ramp test to max) for VO₂peak and fitness (% predicted VO₂peak).
- Cardiac imaging
- Genotyping to calculate HR-PRS (derived from ~13k gene variants)
They defined “resting bradycardia” using a minimum heart rate of ≤40 bpm, where “minimum heart rate” was the lowest sustained heart rate averaged over at least 30 seconds (a key detail—this avoids being fooled by a single brief pause). They also quantified “bradycardia burden” as the percentage of time when someone’s heart rate was <50 bpm, and they tracked pauses (≥2 seconds) and heart rhythm patterns that may be suggestive of heart block.
Follow-up happened about 5 years later via questionnaire and focused on clinically relevant outcomes, including syncope, arrhythmias, device implantation, stroke, and sudden death, with events verified when possible.
So, what did they find?
- 38% of athletes had a minimum heart rate ≤40 bpm, but only 2% had a minimum heart rate ≤30 bpm.
- 25% had pauses ≥2 seconds, but only 3% had pauses ≥3 seconds.
- Second-degree AV heart block showed up in 3% of athletes, and no one had complete heart block.
And the “scary stuff” was almost always boring in context: the pauses were predominantly sinus pauses, asymptomatic, and recorded overnight. The longest reported pause was 5.4 seconds in a 19-year-old cyclist, who experienced no symptoms and only happened at night.
Athletes with low heart rates didn’t look abnormal either. They just looked like stronger versions of athletes without abnormally low heart rates. Compared to the non-bradycardic athletes, the bradycardic group tended to be younger and fitter. For example, their VO₂peak was higher (median ~60 vs ~50 mL/kg/min), and they reported a higher training volume. They also showed more “athlete’s heart” remodeling on imaging, with larger atria and ventricles and a higher left ventricular mass. Minimum heart rate correlated moderately with ventricular size (lower heart rate paired with bigger LV/RV volumes). The right atrium stood out not only as larger in bradycardic athletes but also as an independent predictor of lower minimum heart rate.
Genetics matter independently of fitness
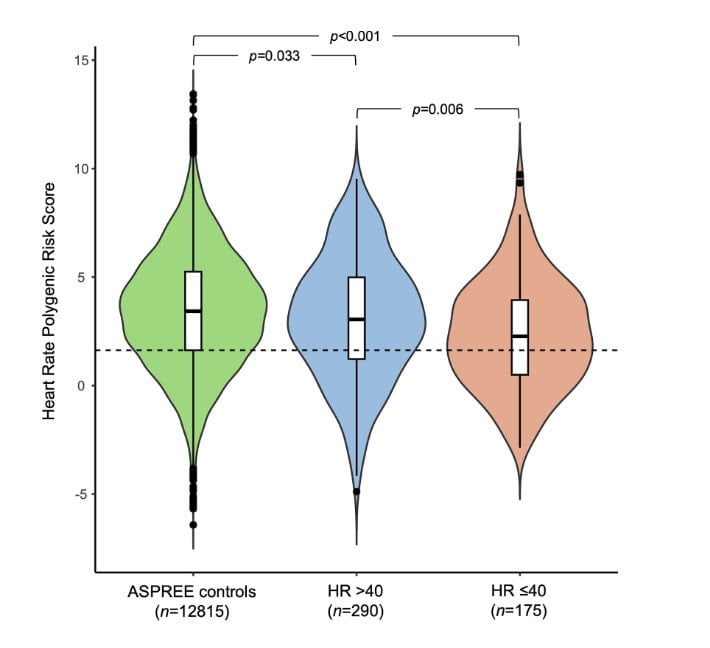
This is the heart of the paper (pun intended): the HR-PRS was lower (more genetically “bradycardia-prone”) in athletes than in nonathletic controls, and lower still in bradycardic athletes.
Within the athlete cohort, those in the lowest HR-PRS quartile had:
- Lower minimum heart rate (median ~41 vs ~45 bpm in the highest quartile)
- A higher bradycardia burden (median ~14% vs ~2% of the day spent <50 bpm)
- More pauses ≥2 seconds (about 36% vs 21%)
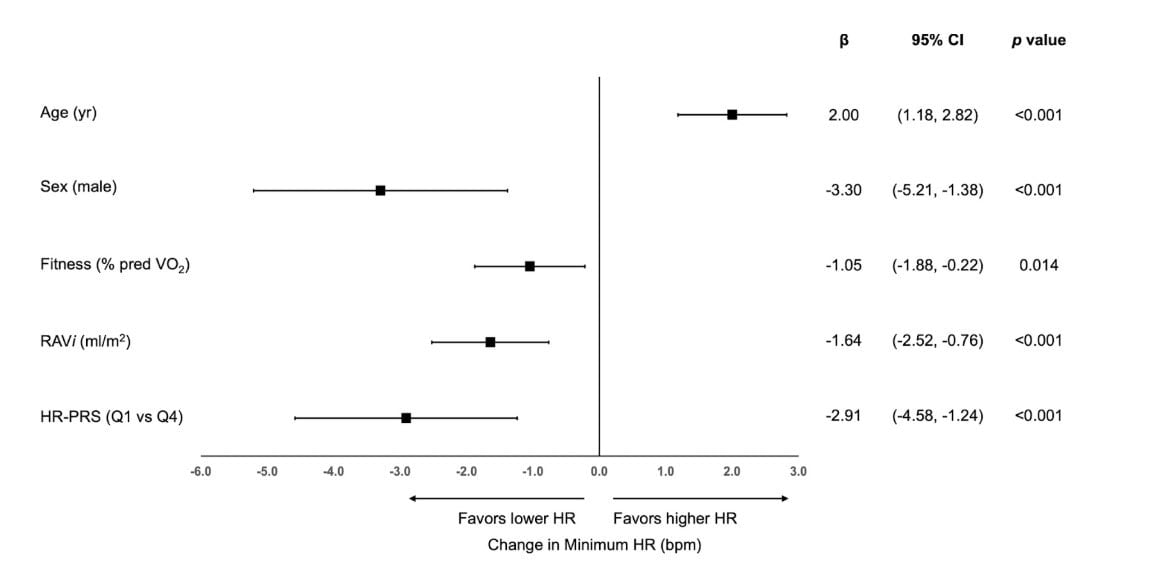
Even after adjusting for age, sex, fitness, and right atrial size, a low HR-PRS was associated with roughly a 2-fold increase in the odds of meeting the “minimum heart rate ≤40” bradycardia definition. In other words, training and fitness mattered, but genetics still explained additional variance that training alone didn’t.
Bradycardia wasn’t linked to worse outcomes
This is the reassuring part for athletes with a low resting heart rate. During the follow-up, syncope (fainting) events were uncommon. Atrial fibrillation occurred, but not in a pattern suggesting that bradycardia itself was the driver. Furthermore, only one athlete (a 76-year-old former rower) got a pacemaker implanted. And among the smaller group with resting heart rates of 30 or below, none experienced fainting, pacemaker implantation, or other adverse outcomes during follow-up.
That doesn’t mean risk is zero—especially across decades—but it strongly pushes back against the idea that bradycardia is a ticking time bomb in otherwise healthy endurance athletes.
Why this matters (and what I think the real takeaway is)
There are two different stories you can tell about athlete’s bradycardia. The traditional story is that endurance training slows the heart through autonomic shifts and sinus node remodeling. The newer, more interesting story is that some people may be genetically biased toward lower heart rates, greater filling, and stronger remodeling—and that biology might make endurance training feel more “compatible,” even before the first training block is finished.
This study doesn’t prove that low-heart-rate genetics causes elite athleticism. But the fact that athletes, as a group, had a more “bradycardia-prone” genetic signature than a healthy reference population raises the possibility that we’re seeing selection at work—the people who end up thriving (and sticking) in endurance sports might be partly those whose baseline physiology is already pointed in that direction.
Of course, this isn’t a perfect paper. It’s mostly cross-sectional (so causality is tricky), and the cohort included a small referral subgroup with known or suspected arrhythmias, which likely inflates the prevalence of atrial fibrillation in the overall sample. The sample was also predominantly male and almost entirely of European ancestry, limiting generalizability. They didn’t measure heart rate variability (so the vagal tone debate remains unresolved), they didn’t capture training load in depth right before testing (overreaching could affect heart rate), and the genetics work focused on common variants, not rare mutations that can matter a lot in individual cases.
What this means for runners
For most well-trained runners, a very low sleeping heart rate, occasional overnight pauses around 2–3 seconds, and even a minimum heart rate in the high 30s can be a normal—and apparently well-tolerated—feature of endurance adaptation, especially when you’re young, aerobically fit, and have no symptoms. The “red flag” threshold (like heart rate <30 bpm or long pauses) appears uncommon even in elite cohorts, and the bigger practical message is that bradycardia isn’t just something you earn, it’s also something you may be predisposed to.
So if your training partner can cruise around with a 34 bpm heart rate while you sit in the mid-40s on the same mileage, that may reflect genetics as much as grit. That may be a frustrating or reassuring conclusion, and it may depend on which side of that heart rate threshold you sit on.
Luckily, they don’t give out medals for who has the lowest resting heart rate.











I have a resting pulse of 35-40 bpm I’m 73 and am a regular runner for over 45 years (marathons, Half marathons, plus a few Ultras) I’ve been checked out several times over the years by Doctors and Cardiologists and they attribute this to the training volume and possibly genetics (my brother has a heart rate of 45 and in good shape but doesn’t work out daily)
So yes, in theory medically I have sinus bradychardia but it doesn’t affect my running …..until recently, when I had a stroke ! Luckily I was treated very quickly (within an hour or so) and have made a full recovery ….very, very lucky. As a result though I’m taking the usual medication to help prevent another.
My reason for saying all this is, it would be interesting to hear the average Blood Pressure of these athletes if possible by age, because I do wonder now from personal experience, how slow powerful heart beats affect Blood pressure and the risk of blood clots forming especially when slightly de hydrated (as runners inevitably are despite drinking during long events ) You’d expect a low resting Blood pressure …but who knows ??